Heel Soreness The Big Causes, Signs And Symptoms And Treatment Choices
Overview

Painful heels are the number 4 concern bringing patients
into the offices of many family doctors and the number one concern bringing patients to the offices of podiatric physicians (foot doctors).
Causes
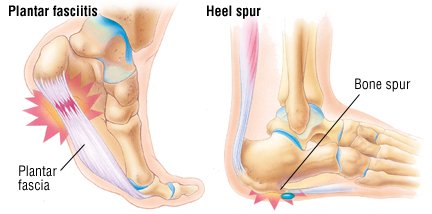
Plantar fasciitis: It is the most common cause of heel pain. In this condition, the pain is more severe in the morning but becomes less painful as the day continues. It occurs due to tiny tears in the plantar fascia.The plantar faschia is a tissue band that connects the bottom of the heel bones to the ball of the foot and is involved in walking and running, giving spring to the step. If left untreated, the symptoms usually worsen and can lead to problems with the knee and hip and can cause back pain due to difficulty walking. Those who frequently stand or walk throughout the day or those who run are most likely to develop plantar fasciitis.
Symptoms
Pain typically comes on gradually, with no injury to the affected area. It is frequently triggered by wearing a flat shoe, such as flip-flop sandals. Flat footwear may stretch the plantar fascia to such an extent that the area becomes swollen (inflamed). In most cases, the pain is under the foot, toward the front of the heel. Post-static dyskinesia (pain after rest) symptoms tend to be worse just after getting out of bed in the morning, and after a period of rest during the day. After a bit of activity symptoms often improve a bit. However, they may worsen again toward the end of the day.
Diagnosis
After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including. Whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Your doctor will examine you, including. An evaluation of your gait. While you are barefoot, your doctor will ask you to stand still and to walk in order to evaluate how your foot moves as you walk. An examination of your feet. Your doctor may compare your feet for any differences between them. Then your doctor may examine your painful foot for signs of tenderness, swelling, discoloration, muscle weakness and decreased range of motion. A neurological examination. The nerves and muscles may be evaluated by checking strength, sensation and reflexes. In addition to examining you, your health care professional may want to examine your shoes. Signs of excessive wear in certain parts of a shoe can provide valuable clues to problems in the way you walk and poor bone alignment. Depending on the results of your physical examination, you may need foot X-rays or other diagnostic tests.
Non Surgical Treatment
Treatment of heel pain generally occurs in stages. At the earliest sign of heel pain, aggressive calf muscle stretching should be started. Additionally, taking an oral anti-inflammatory medication and over-the- counter arch supports or heel cushions may be beneficial. The next phase of treatment might consist of continued calf muscle stretching exercises, cortisone injections and orthopedic taping of the foot to support the arch. If this treatment fails, or if there is reoccurrence of the heel pain, then functional foot orthotics might be considered. A functional orthotic is a device that is prescribed and fitted by your foot doctor, which fits in normal shoes like an arch support. Unlike an arch support, however the orthotic corrects abnormal pronation of the subtalar joint. Thus orthotics address the cause of the heel pain - abnormal pronation of the foot. Pump bump, treatment is similar to the treatment of bursitis and heel spurs. In rare cases, the bony growth at the heel may need to be removed surgically. Heel bruises can be treated by applying an ice pack for the first few minutes after injury. Achilles tendonitis, this condition is treated conservatively with rest, NSAIDs and physical therapy. If a sprain, fracture or other injury has caused the trapped nerve, this underlying problem must be treated first. In rare cases, surgery may be done to release the trapped nerve.
Surgical Treatment
Surgery to correct heel pain is generally only recommended if orthotic treatment has failed. There are some exceptions to this course of treatment and it is up to you and your doctor to determine the most appropriate course of treatment. Following surgical treatment to correct heel pain the patient will generally have to continue the use of orthotics. The surgery does not correct the cause of the heel pain. The surgery will eliminate the pain but the process that caused the pain will continue without the use of orthotics. If orthotics have been prescribed prior to surgery they generally do not have to be remade.
heel pads shoes too big
Prevention
You can reduce the risk of heel pain in many ways, including. Wear shoes that fit you properly with a firm fastening, such as laces. Choose shoes with shock-absorbent soles and supportive heels. Repair or throw out any shoes that have worn heels. Always warm up and cool down when exercising or playing sport, include plenty of slow, sustained stretches. If necessary, your podiatrist will show you how to tape or strap your feet to help support the muscles and ligaments. Shoe inserts (orthoses) professionally fitted by your podiatrist can help support your feet in the long term.

Painful heels are the number 4 concern bringing patients
into the offices of many family doctors and the number one concern bringing patients to the offices of podiatric physicians (foot doctors).
Causes
Plantar fasciitis: It is the most common cause of heel pain. In this condition, the pain is more severe in the morning but becomes less painful as the day continues. It occurs due to tiny tears in the plantar fascia.The plantar faschia is a tissue band that connects the bottom of the heel bones to the ball of the foot and is involved in walking and running, giving spring to the step. If left untreated, the symptoms usually worsen and can lead to problems with the knee and hip and can cause back pain due to difficulty walking. Those who frequently stand or walk throughout the day or those who run are most likely to develop plantar fasciitis.
Symptoms
Pain typically comes on gradually, with no injury to the affected area. It is frequently triggered by wearing a flat shoe, such as flip-flop sandals. Flat footwear may stretch the plantar fascia to such an extent that the area becomes swollen (inflamed). In most cases, the pain is under the foot, toward the front of the heel. Post-static dyskinesia (pain after rest) symptoms tend to be worse just after getting out of bed in the morning, and after a period of rest during the day. After a bit of activity symptoms often improve a bit. However, they may worsen again toward the end of the day.
Diagnosis
After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including. Whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Your doctor will examine you, including. An evaluation of your gait. While you are barefoot, your doctor will ask you to stand still and to walk in order to evaluate how your foot moves as you walk. An examination of your feet. Your doctor may compare your feet for any differences between them. Then your doctor may examine your painful foot for signs of tenderness, swelling, discoloration, muscle weakness and decreased range of motion. A neurological examination. The nerves and muscles may be evaluated by checking strength, sensation and reflexes. In addition to examining you, your health care professional may want to examine your shoes. Signs of excessive wear in certain parts of a shoe can provide valuable clues to problems in the way you walk and poor bone alignment. Depending on the results of your physical examination, you may need foot X-rays or other diagnostic tests.
Non Surgical Treatment
Treatment of heel pain generally occurs in stages. At the earliest sign of heel pain, aggressive calf muscle stretching should be started. Additionally, taking an oral anti-inflammatory medication and over-the- counter arch supports or heel cushions may be beneficial. The next phase of treatment might consist of continued calf muscle stretching exercises, cortisone injections and orthopedic taping of the foot to support the arch. If this treatment fails, or if there is reoccurrence of the heel pain, then functional foot orthotics might be considered. A functional orthotic is a device that is prescribed and fitted by your foot doctor, which fits in normal shoes like an arch support. Unlike an arch support, however the orthotic corrects abnormal pronation of the subtalar joint. Thus orthotics address the cause of the heel pain - abnormal pronation of the foot. Pump bump, treatment is similar to the treatment of bursitis and heel spurs. In rare cases, the bony growth at the heel may need to be removed surgically. Heel bruises can be treated by applying an ice pack for the first few minutes after injury. Achilles tendonitis, this condition is treated conservatively with rest, NSAIDs and physical therapy. If a sprain, fracture or other injury has caused the trapped nerve, this underlying problem must be treated first. In rare cases, surgery may be done to release the trapped nerve.
Surgical Treatment
Surgery to correct heel pain is generally only recommended if orthotic treatment has failed. There are some exceptions to this course of treatment and it is up to you and your doctor to determine the most appropriate course of treatment. Following surgical treatment to correct heel pain the patient will generally have to continue the use of orthotics. The surgery does not correct the cause of the heel pain. The surgery will eliminate the pain but the process that caused the pain will continue without the use of orthotics. If orthotics have been prescribed prior to surgery they generally do not have to be remade.
heel pads shoes too big
Prevention

You can reduce the risk of heel pain in many ways, including. Wear shoes that fit you properly with a firm fastening, such as laces. Choose shoes with shock-absorbent soles and supportive heels. Repair or throw out any shoes that have worn heels. Always warm up and cool down when exercising or playing sport, include plenty of slow, sustained stretches. If necessary, your podiatrist will show you how to tape or strap your feet to help support the muscles and ligaments. Shoe inserts (orthoses) professionally fitted by your podiatrist can help support your feet in the long term.